And somehow it’s already May. Happy Celiac Awareness Month!
To celebrate, here’s a roundup of research on Celiac & digestive conditions, with some resources & recipes below. And I know some of the links look like they’re broken, but they work.

- Gluten-related disorders from bench to bedside—a wide ranging review on Celiac, gluten sensitivity and wheat allergy from AGA
- Which is the chicken, which is the egg? We know many people with celiac have low iron. But can iron supplementation prevent celiac?
- Celiac & IBS are associated. Someone with Celiac is more likely to be diagnosed with IBS than someone in the general population, and siblings are more likely to receive an IBS diagnosis, too.
- New study in BMJ show exercise is great for mood. If for some reason it’s not possible and/or not in your best interest, there are absolutely other good ways to take care of your mental health.
- New pesticide residue calculator:
- A quiz on some of the latest Celiac research. How will you do?
- A homemade enteral formula for pediatric Crohn’s? Fascinating new research…
- A lot of people with IBD still have persistent symptoms and pain. What to do? More here:
We’re about to roll into the best time of year for trips, travel & time on the go. A list of grab and go gluten-free foods is here.
Here are some veggie-based recipes for some (gluten-free) and lighter summertime recipes.
Hope you enjoy the rest of the beautiful weather.
Cheryl Harris, MPH, RD is a Registered Dietitian Nutritionist and Certified Wellcoach working with clients in VA, DC & MD. She helps people with a range of digestive problems, including Celiac, IBS, Crohn’s, UC, gastroparesis, EDS, POTS & more. Let’s get you on your way to achieving your goals and feeling great! Email or call 571-271-8742.

 How…did November fly by so fast?
How…did November fly by so fast?
 Health, and sometimes they make an appearance for sessions. They’re originally from Ukraine–their names are Myshko and Zhanna. They lost their homes in the conflict, so they’ve come to live with us. When they’re awake, they’ve taken over our house, and are completely running the show. They have strong feelings about omega 3s and occasionally you’ll see a tail flying by.
Health, and sometimes they make an appearance for sessions. They’re originally from Ukraine–their names are Myshko and Zhanna. They lost their homes in the conflict, so they’ve come to live with us. When they’re awake, they’ve taken over our house, and are completely running the show. They have strong feelings about omega 3s and occasionally you’ll see a tail flying by.



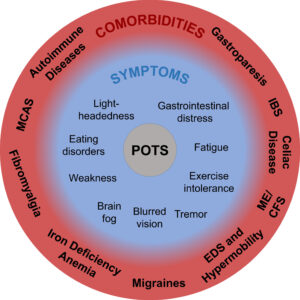 Ever heard of POTS (Postural Orthostatic Tachycardia Syndrome?) Too few people have. It’s fairly common, and before COVID, it affected around 1% of the population. I got POTS when I was in grad school, and it’s always been on my radar because 4% of people with POTS have Celiac, instead of the usual 1%, and ~95% of people have digestive issues. Since COVID, rates of POTS have increased significantly because it’s often post viral. I have a paper on the nutritional management of POTS in the
Ever heard of POTS (Postural Orthostatic Tachycardia Syndrome?) Too few people have. It’s fairly common, and before COVID, it affected around 1% of the population. I got POTS when I was in grad school, and it’s always been on my radar because 4% of people with POTS have Celiac, instead of the usual 1%, and ~95% of people have digestive issues. Since COVID, rates of POTS have increased significantly because it’s often post viral. I have a paper on the nutritional management of POTS in the  Passover isn’t here until April 15th but many of the products are already appearing in grocery stores. Not all Passover foods are gluten-free, but many are, and there’s a much wider selection than usual at the grocery store. This can be a good time to stock up on GF cakes and mixes, cookies, macaroons, some of the “bread” crumbs and supplies like potato starch. As an added bonus for people with multiple restrictions, most Kosher for Passover products contain no corn or soy products, either.
Passover isn’t here until April 15th but many of the products are already appearing in grocery stores. Not all Passover foods are gluten-free, but many are, and there’s a much wider selection than usual at the grocery store. This can be a good time to stock up on GF cakes and mixes, cookies, macaroons, some of the “bread” crumbs and supplies like potato starch. As an added bonus for people with multiple restrictions, most Kosher for Passover products contain no corn or soy products, either.
 Toasted Sugar Almond and Hazelnut Meringues, above, (using
Toasted Sugar Almond and Hazelnut Meringues, above, (using 
 portions in the Monash app just don’t jive with what I’ve found with clients. Well…
portions in the Monash app just don’t jive with what I’ve found with clients. Well…
